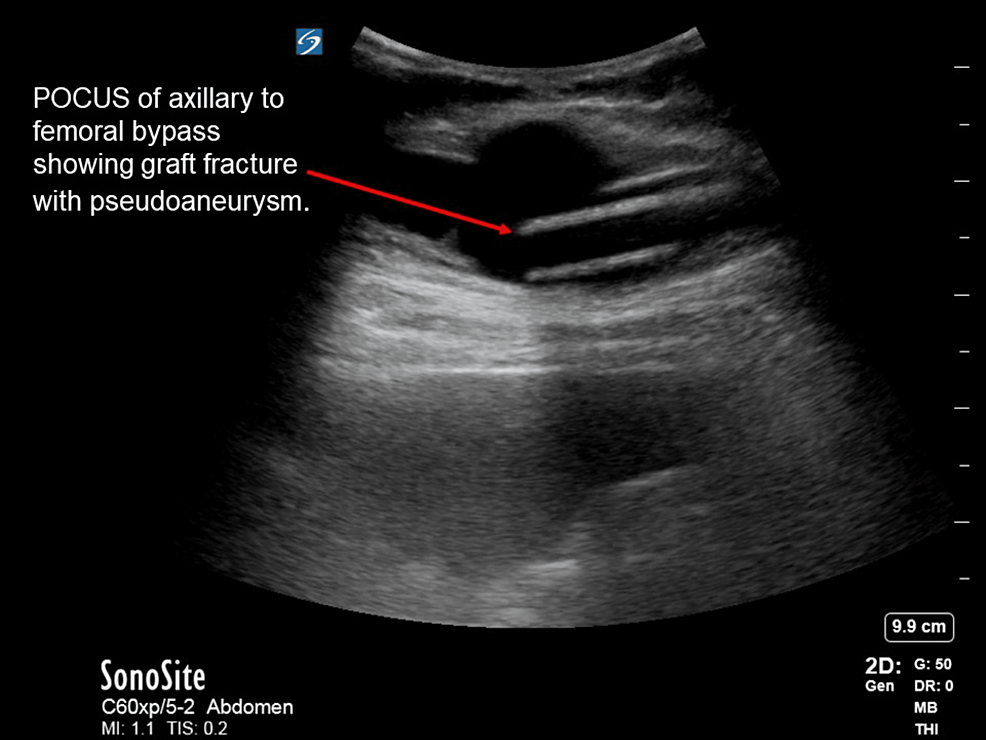
Bi-femoral axillary bypass graft placement is a well-known and typically safe procedure. It is generally indicated for patients with advanced peripheral vascular disease, aortoiliac occlusive disease, or infectious artery disease. In rare cases, the graft can be fractured or dislodged after placement, though most often, this occurs almost exclusively at the anastomosis site, secondary to blunt trauma. Using ultrasonic imaging is a reliable method of detecting these fractures. We present a case of a bi-femoral axillary bypass graft fracture in a 68-year-old male with the development of a pseudoaneurysm in the right lateral abdominal wall. The patient reported spontaneous development of a “strange” sensation in his right lower abdomen and a “painful lump” upon waking. Physical examination showed a small right lower quadrant outpouching which was pulsatile on palpation. The initial workup included a bedside ultrasound which showed a fractured graft with the fluid collection and a Doppler signal. Vascular surgery was immediately consulted for evaluation, and the patient was taken to the operating room for emergent surgical repair. CT angiography confirmed a successful operation in which an 8 mm graft was placed to anastomose the original bypass graft fracture site. The patient remained stable postoperatively and was discharged without further complications. This report highlights the importance of using ultrasonography for the immediate identification of potential graft complications to prevent serious complications and expedite definitive management.
Introduction
Polytetrafluoroethylene (PTFE) grafts have been used by vascular surgeons for decades to improve blood flow in patients that suffer from conditions that occlude or otherwise impair their native circulatory systems [1]. Of particular interest, in this case, is the bi-femoral axillary bypass (BiFAXB) graft which is performed on patients with peripheral vascular disease, aortoiliac occlusive…